Your Blood Pressure Pill May Be Solving the Wrong Problem
A new study published in April 2026 in Circulation Research – one of the world’s top cardiovascular journals has quietly shaken the foundations of how scientists understand high blood pressure. Researchers from the University of São Paulo, Brazil and the University of Auckland, New Zealand have identified a tiny region deep inside your brainstem that may be directly responsible for spiking blood pressure in millions of patients. And here is the part that should make every hypertension patient in India pause, this brain region has nothing to do with your heart, kidneys, or salt intake. According to the World Health Organization, over 220 million Indians currently live with hypertension. Many of them take medication every day. Many of them are still not in control.
The Brain Region Nobody Was Watching
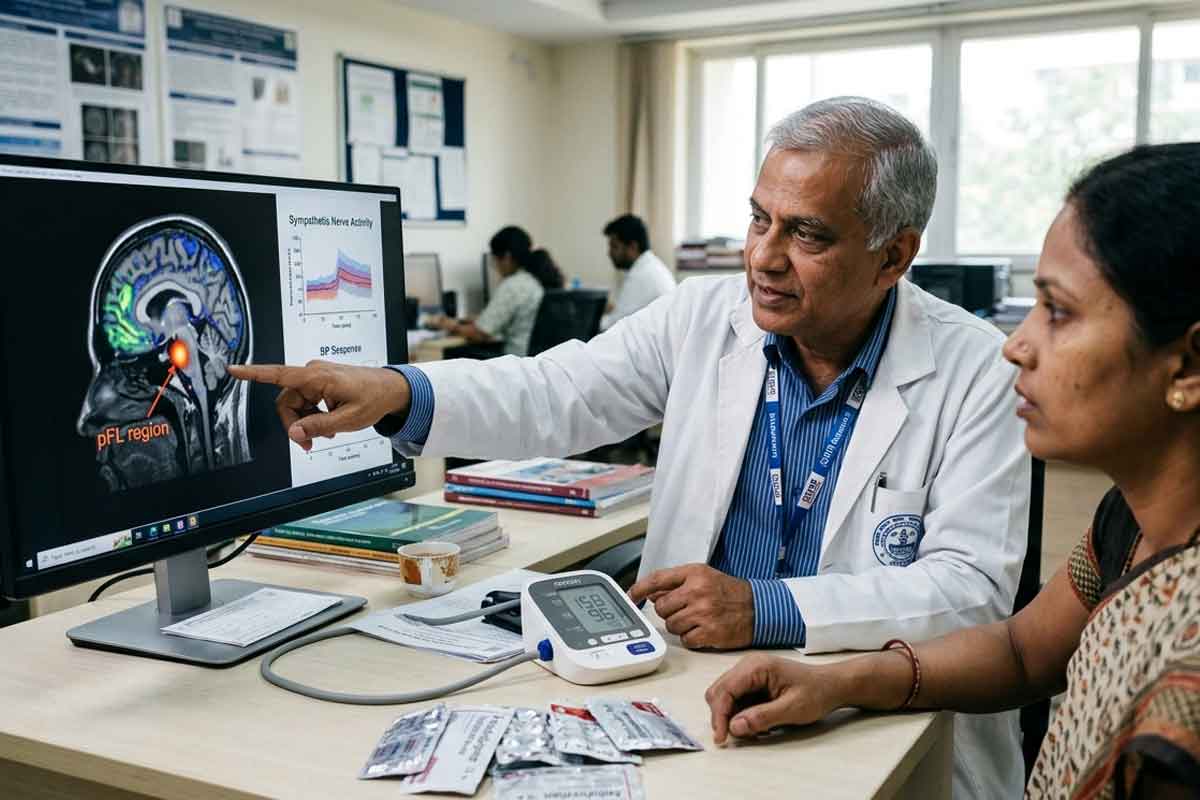
The region in question is called the lateral parafacial region, or pFL for short. It sits in the medulla oblongata, the lowest part of the brainstem, the ancient part of your brain that handles automatic functions like breathing, digestion, and heart rate. Until recently, scientists believed the pFL had one job: controlling forceful exhalation. That kind of exhale happens when you cough, laugh hard, sneeze, or push through the last rep at the gym.
What nobody expected was that this same region also sends signals to nerves that tighten blood vessels. Lead researcher Professor Julian Paton, Director of Manaaki Manawa Centre for Heart Research at the University of Auckland, put it plainly: “We’ve unearthed a new region of the brain that is causing high blood pressure. Yes, the brain is to blame for hypertension.”
In experiments using rats, the team used a technique called viral transfection, where modified viruses reprogram specific neurons to switch pFL neurons on and off. When they activated the pFL region, blood pressure rose. When they silenced it, blood pressure in hypertensive rats fell back to normal levels. That last part is the breakthrough. Not just finding the cause but showing you can reverse it.
Why 40% of Patients Are Still Failing Their Treatment?
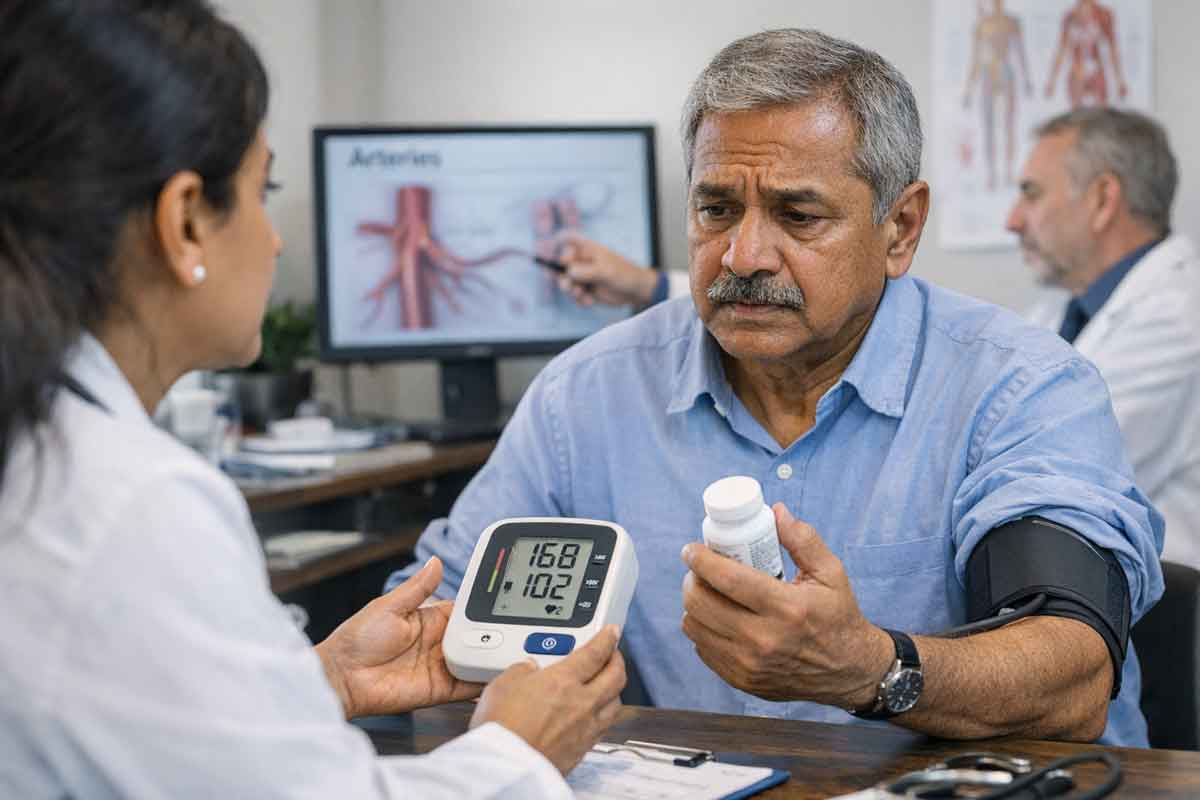
Here is a number that rarely gets discussed openly. According to the study’s own findings, approximately 40% of patients currently on blood pressure medication remain hypertensive meaning their BP is still not under control despite taking prescribed drugs. For years, doctors have called this “resistant hypertension” and often blamed patient compliance. Were they eating too much salt? Skipping doses?
This research offers a different explanation. Around 50% of all hypertension cases have a neurogenic component, meaning the problem originates in the nervous system, not just the cardiovascular system. If your hypertension is driven by an overactive pFL region firing sympathetic nerve signals, then an ACE inhibitor targeting your blood vessels is not going to fix the root problem. It is treating downstream effects, not the actual source.
Think about it this way. If a pipe keeps bursting because the water pressure valve is broken, you can keep patching the pipe or you can fix the valve. Most current hypertension drugs are very good at patching the pipe.
Sleep Apnea Connection That Affects Crores of Indians
This finding also unlocks something that has puzzled doctors for years, why do people with obstructive sleep apnea (OSA) have significantly higher rates of hypertension?
The pFL neurons do not fire during normal, relaxed breathing. But when oxygen levels drop or CO2 rises exactly what happens when someone stops breathing momentarily during sleep apnea the pFL region activates. It then triggers sympathetic nerve activity, which constricts blood vessels and raises blood pressure. Every night. Repeatedly. Without the person being aware.
In India, OSA is severely underdiagnosed. Most families chalk up loud snoring to fatigue or sleeping position. The Indian Journal of Medical Research has estimated that OSA prevalence in India may be as high as 13.7% in men and 5% in women but treatment rates remain very low. If you or someone at home snores heavily and also has high blood pressure that is difficult to control, this connection is worth taking seriously with a doctor.
Myth That Needs to Go: “High BP Is a Heart Problem”
Most Indians and many general physicians, think of hypertension as primarily a heart-and-kidney issue. Eat less salt, lose weight, take your pill. That advice is not wrong. But it is incomplete.
The pFL research confirms what neurologists have suspected for some time, the brain is an active participant in blood pressure regulation, not a passive bystander. The sympathetic nervous system your body’s fight-or-flight response plays a direct role in keeping blood vessels constricted. And the brain is the one pulling those strings. Treating hypertension only at the organ level, while ignoring the neural signals driving it, is why so many patients plateau on medication.
How the New Treatment Approach Would Work?
Targeting the brain directly with drugs is complicated medicines tend to act on the entire brain, not one specific nucleus. But the researchers found an elegant workaround. The pFL region receives signals from carotid bodies — small clusters of cells located near the carotid arteries in your neck. These act like oxygen sensors. When oxygen drops, carotid bodies alert the pFL, which then activates sympathetic nerve activity.
By targeting the carotid bodies with drugs from outside the brain, it may be possible to calm the pFL region indirectly. The team is now working on identifying compounds that block the relevant ATP receptors in the carotid bodies. This is still in early research phase and has only been tested in animal models so far. Human trials are the critical next step.
| Factor | Current Hypertension Drugs | pFL / Neurogenic Approach (Research Stage) |
|---|---|---|
| Target Organ | Heart, kidneys, blood vessels | Brainstem / carotid bodies |
| Mechanism | Reduce cardiac output, dilate vessels, remove fluid | Suppress sympathetic nerve overactivity at source |
| Works For | Most hypertension types | Neurogenic hypertension (~50% of cases) |
| Limitation | Fails in ~40% of resistant cases | Still in animal model phase, not yet human-approved |
| Sleep Apnea Link | Not directly addressed | Directly explains and targets this connection |
| India Availability | Widely available, Rs 10–200/month | Not yet available, years from clinical use |
Did Ancient Breathing Practices Already Know This?
Here is something no Western science journal will write, but it is worth asking. Pranayama, the ancient Indian system of breath control has long emphasized slow, controlled exhalation as central to cardiovascular and nervous system health. Practices like Anulom Vilom and Bhramari directly train the exhale to be smooth, prolonged, and controlled the exact opposite of the forceful abdominal exhale that activates the pFL region.
A 2021 study in the Journal of Hypertension found that slow breathing exercises reduced systolic blood pressure by an average of 8–10 mmHg over 8 weeks. At the time, researchers were not sure why the effect was so significant. The pFL discovery may now offer a neurological explanation: controlled breathing reduces the forceful exhalation pattern that triggers pFL activation, thereby reducing sympathetic nerve output and blood pressure. This is still a hypothesis but it is a scientifically grounded one.
What You Should Do With This Information Right Now?
This research is not a reason to stop your current blood pressure medication. That would be dangerous. But it is a very good reason to have a more informed conversation with your doctor. Here is what is actually actionable today:
- If your BP is not controlled despite medication – ask your doctor about a neurogenic component evaluation. Mention this study (Circulation Research, 2026, Magalhães et al.) specifically.
- If you or a family member snores heavily – request a sleep study or at minimum discuss OSA screening at your next appointment. In cities like Delhi, Mumbai, Bangalore, and Hyderabad, sleep clinics are widely available at major hospitals.
- If you want to add a complementary approach – slow breathing exercises (4-count inhale, 6-8 count exhale) for 10–15 minutes daily have evidence behind them. This costs nothing and has no side effects.
- Do not self-diagnose neurogenic hypertension – the tools to confirm this do not yet exist in standard clinical settings. This research is pointing toward a future diagnostic, not a current one.
The brain’s role in blood pressure is not a fringe theory anymore. It is peer-reviewed science published in one of cardiology’s most respected journals. The drugs that help millions of Indians every day are not obsolete but they may soon have a smarter partner in treatment. That is genuinely good news for the 220 million who need it.
FAQ
Q. Is this brain-based hypertension treatment available in India right now?
No, not yet. The pFL research has only been tested in animal models so far. Human clinical trials are the next step, which typically take several years. Current approved medications remain the standard of care. This discovery is important for the future of treatment, not an immediate replacement for what your doctor has prescribed.
Q. How do I know if my hypertension has a neurogenic component?
Right now, there is no standard clinical test available to confirm neurogenic hypertension in regular hospital settings. The clearest sign is BP that remains uncontrolled despite taking two or more medications as prescribed. If that is your situation, ask your cardiologist or physician about further evaluation. OSA screening is a good starting point, since the sleep apnea–pFL connection is now well-supported by research.
Q. Can slow breathing exercises actually lower blood pressure?
Yes, there is solid evidence for this. Studies including one published in the Journal of Hypertension show that practising slow, controlled breathing (especially longer exhales) for 10–15 minutes a day can reduce systolic blood pressure by 8–10 mmHg over several weeks. This is not a replacement for medication but a meaningful complement to it. The new pFL research may explain exactly why the exhale pattern matters so much neurologically.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. The pFL brain research cited is based on animal models and has not yet been validated in human clinical trials. Do not stop, reduce, or change your blood pressure medication based on this article. Always consult a qualified medical professional for diagnosis and treatment decisions related to hypertension or any other health condition.
Written by: Anil Sinha – News Hours18






